Exploring the true future of medical simulation training
Have you ever stopped to consider how doctors will actually learn their complex surgical and diagnostic craft a decade from now? The traditional classroom lecture, heavily reliant on static textbooks, is rapidly becoming obsolete.
If we look closely at the future of medical simulation training, it is defined by the complete integration of artificial intelligence and hyper-realistic manikins. This cohesive technological ecosystem allows practitioners to practice incredibly complex procedures without ever risking actual human lives.
The simulation technology advancements healthcare professionals rely on today are merely the foundation. We are entering a dynamic, responsive educational era that completely redefines clinical preparation.
Are virtual environments replacing physical care models?
It is incredibly tempting to think that virtual reality will eventually replace physical hardware entirely. You simply put on a digital headset, grab some plastic controllers, and suddenly you are standing inside a fully functioning trauma bay.
However, the reality of emerging technologies in medical education simulation points to a much more integrated, hybrid approach. Visual fidelity is fantastic for spatial awareness, but a surgeon still fundamentally needs to feel the genuine physical resistance of human tissue.
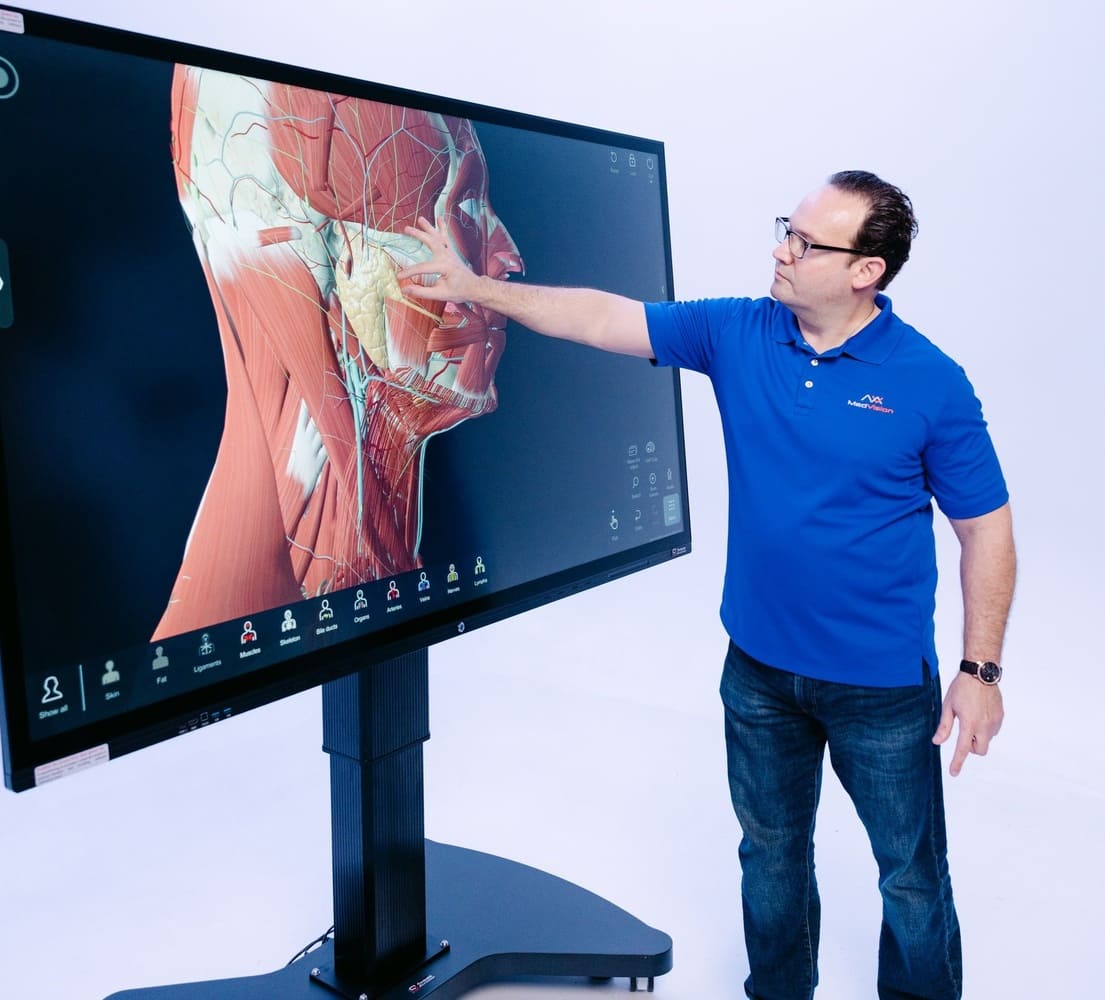
This is exactly why the industry focuses on interconnected, tactile systems. You might study complex internal anatomical structures using a digital SVision 3D Anatomy Table from MedVision, but you still absolutely need a high-fidelity physical model to practice deep chest compressions.
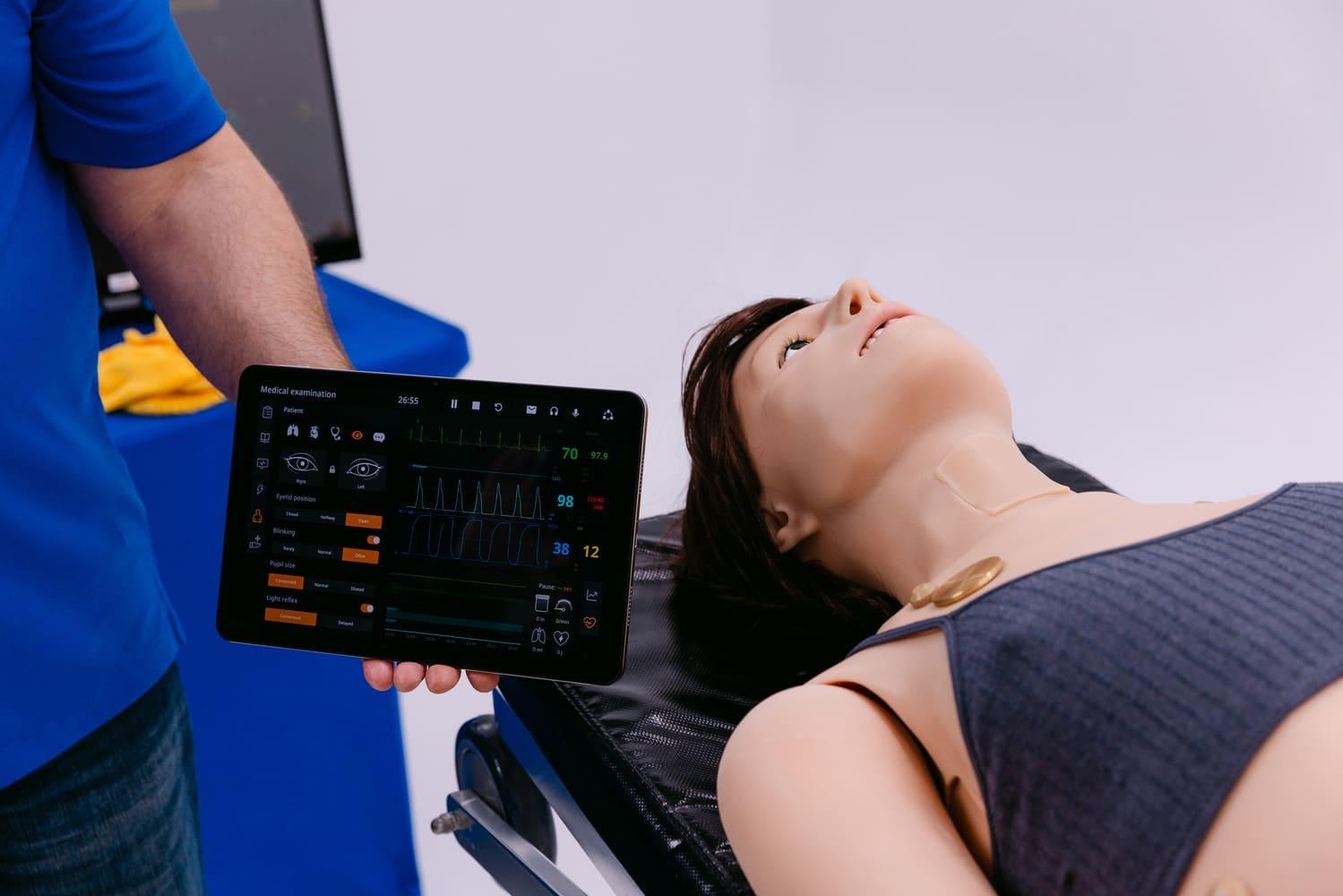
The true future of this specific training lies in seamlessly blending these two distinct worlds. A medical student might wear augmented reality glasses while interacting directly with a physical Leonardo adult patient simulator. They will literally see digital blood pressure metrics floating dynamically above a tangible chest.
How will AI manipulate complex healthcare scenarios?
Right now, the vast majority of educational scenarios are rigidly pre-programmed by human instructors. An educator sits behind a two-way mirror in a control room and manually triggers a sudden cardiac arrest or a massive hemorrhage.
But what happens when the software practically runs itself using advanced machine learning? Artificial intelligence is the ultimate game-changer for any modern clinical simulation center. We are rapidly moving toward predictive algorithms that instantly analyze a student's live performance.
AI manipulates simulation software to alter the clinical scenario on the fly, testing specific, hidden weaknesses. If a nursing student consistently struggles with calculating pediatric medication dosages under time constraints, the AI will immediately recognize this mathematical flaw.
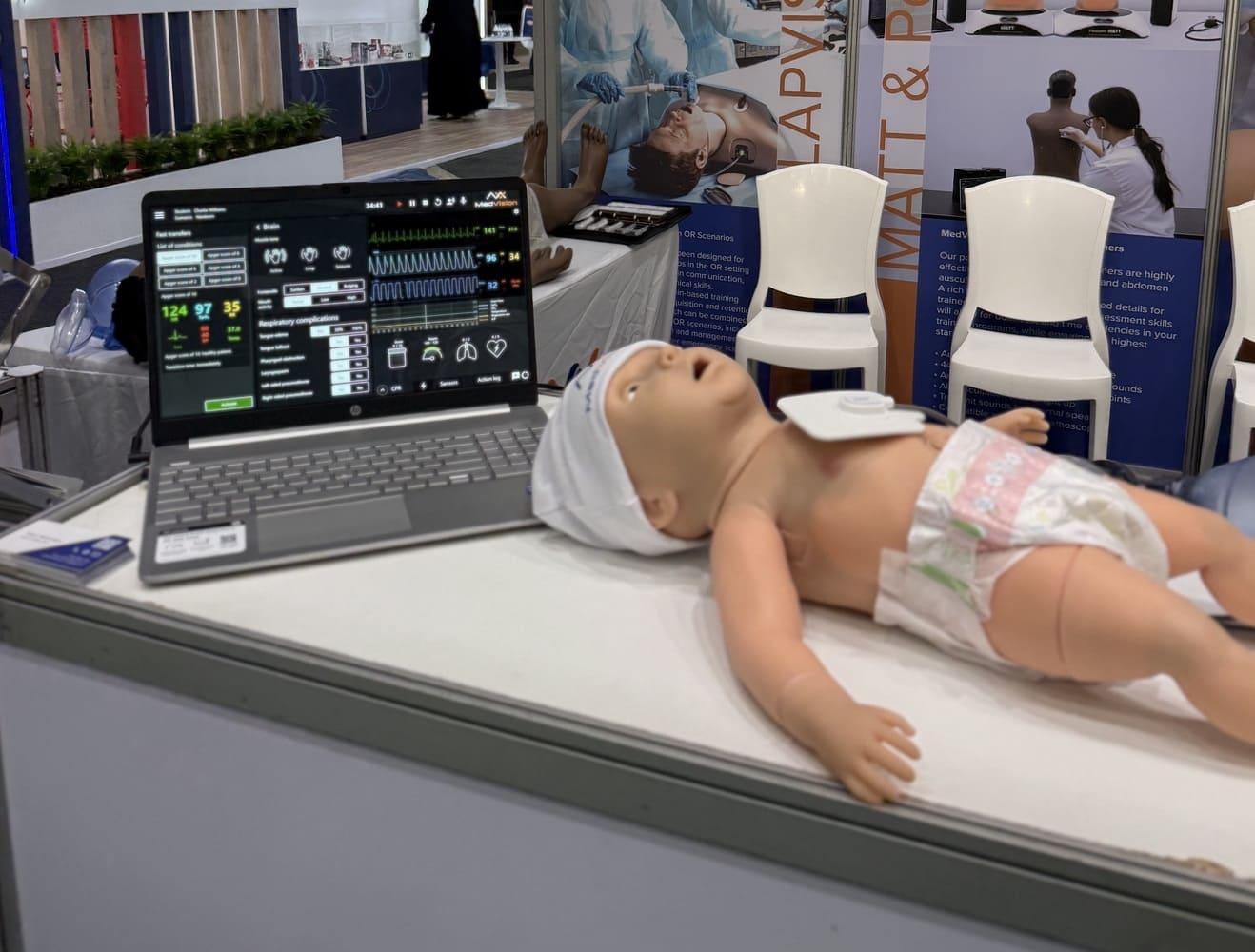
During their next session with the Mia infant simulator, the software will organically generate a chaotic scenario that specifically demands complex pharmacological math. This level of hyper-personalized training was completely impossible just five years ago.
It guarantees that every single healthcare professional receives highly targeted, individualized instruction that continuously adapts to their personal learning curve.
What role does big data play in shaping industry trends?
We generate an unfathomable amount of raw, granular data every single time a medical team runs a code blue drill. Historically, most of that incredibly valuable data was simply ignored after a quick verbal debriefing.
But the latest simulation technology advancements healthcare administrators are adopting focus heavily on deep, algorithmic analytics. Every single breath, every applied joule of electricity, and the exact depth of every chest compression is logged and analyzed.
By aggregating this massive volume of performance data across hundreds of sessions, universities can quickly identify systemic, hidden flaws in their curriculums. Are sixty percent of your third-year surgical residents failing to recognize the early physiological signs of sepsis?
The aggregated data will reveal this dangerous blind spot immediately. This allows clinical educators to adapt their training protocols proactively rather than reactively. Medical trends will no longer be dictated by historical guesswork, but by hard, undeniable performance metrics.
Is decentralized healthcare education the new normal?
Recent global disruptions forced the medical community to completely rethink how we deliver critical clinical education. You cannot always safely or economically gather fifty medical students in a single university lecture hall.
The future of medical simulation training heavily incorporates remote, cloud-based learning infrastructure and high-speed connectivity. Imagine an expert, world-renowned surgeon sitting in London, looking at a live digital feed.
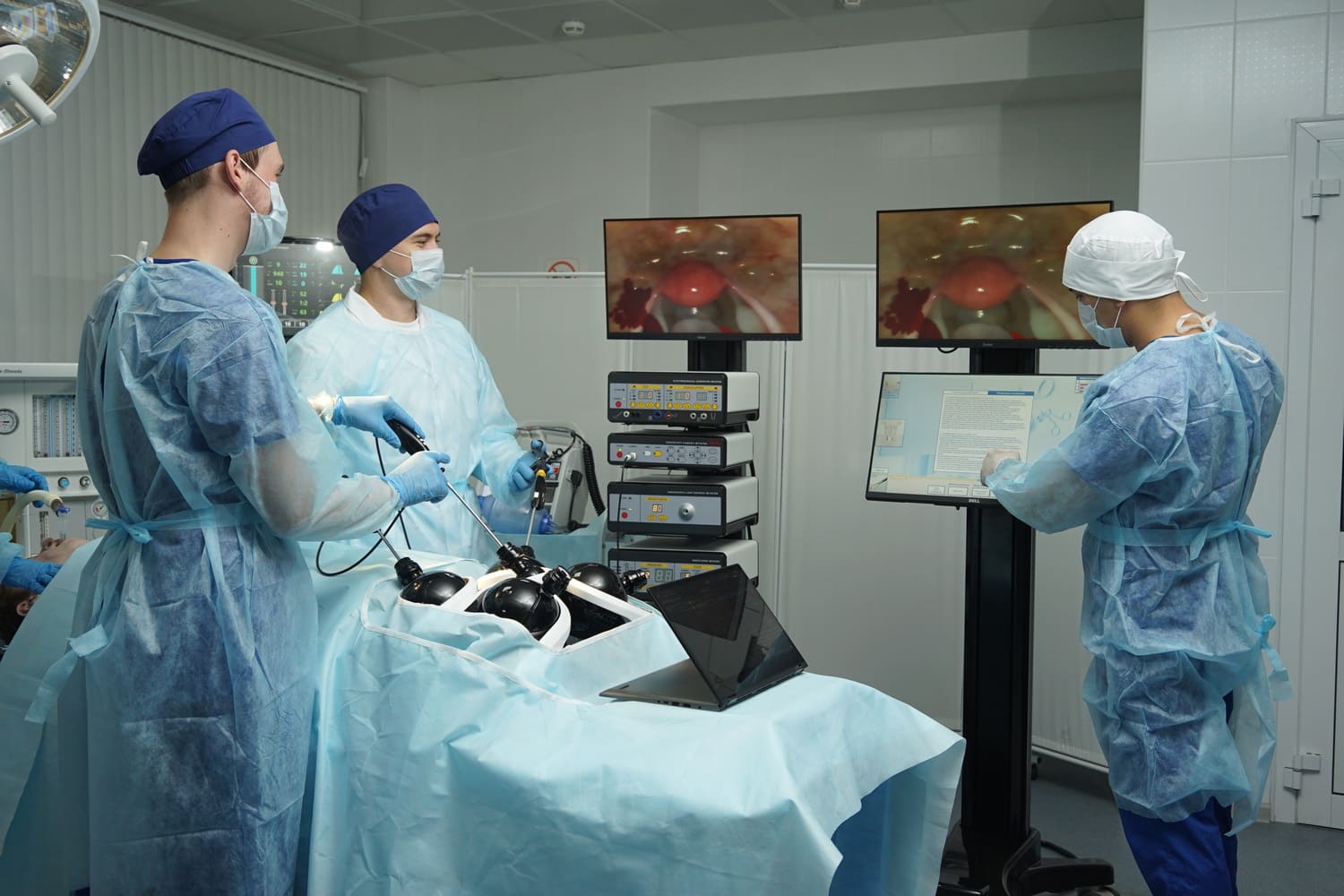
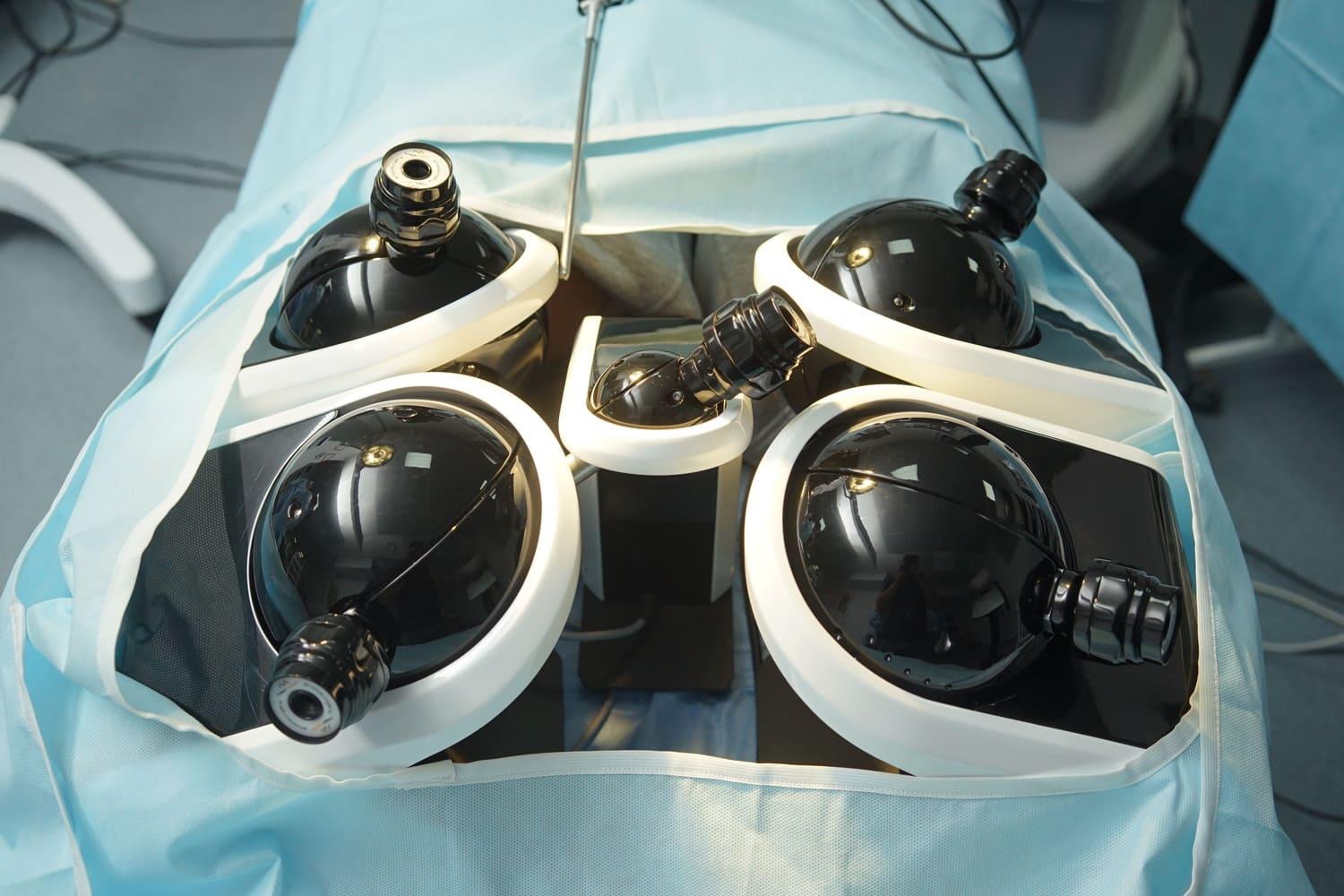
Using advanced networking, they can virtually step into a simulation operating room in New York and actively guide a local resident through a complex laparoscopic procedure using systems like LapVision.
This digital interconnectedness breaks down physical geographical barriers entirely. A small, underfunded rural clinic can now access the exact same high-level scenarios used by top-tier, globally recognized academic hospitals.
Instructors can seamlessly monitor live video feeds, manipulate vital signs remotely, and conduct comprehensive debriefings via secure cloud platforms. This ensures that every single healthcare provider receives access to world-class training methodologies.
Will physical manikins ever feel perfectly human?
Despite all the incredible digital software upgrades, the physical realism of the hardware remains a massive, non-negotiable priority. When you touch a synthetic arm to find a deep, rolling vein, it needs to feel exactly like human skin and muscle.
We are seeing incredible, rapid advancements in polymer sciences and complex haptic feedback mechanisms. Future physical simulation models will actually sweat, and their synthetic tissue will accurately mimic the density of real healthanomalies, such as tumors.
Think about highly specialized surgical training. A platform like HystVision or AngioVision relies entirely on precise, microscopic tactile feedback. If the internal wire resistance feels even slightly artificial, the surgeon learns the wrong muscle memory.
The continuous engineering push for hyper-realism ensures that when a healthcare professional finally transitions from a lab environment to a live human patient, their hands already know exactly what to do. There is zero hesitation.
Why are hospitals bringing the simulation directly to the ward?
For a very long time, clinical labs were hidden away in hospital basements. You had to physically schedule time, leave your busy department, and walk down to an isolated, quiet room. The modern educational approach is completely different.
We are seeing a massive, industry-wide shift toward in-situ clinical training. This means bringing mobile, high-fidelity equipment directly into the actual, chaotic working environment of the hospital ward.
Imagine a surgical team running a massive hemorrhage drill inside their own operating room, using their actual crash carts and monitors alongside a realistic Lisa adult female simulator. This process exposes hidden, latent safety threats within the workspace itself.
References & Literature
- Issenberg, S. B., McGaghie, W. C., Petrusa, E. R., Lee Gordon, D., & Scalese, R. J. (2005). "Features and uses of high-fidelity medical simulations that lead to effective learning: a BEME systematic review." Medical Teacher, 27(1), 10-28.
- Gaba, D. M. (2004). "The future vision of simulation in health care." Quality and Safety in Health Care, 13(suppl 1), i2-i10.
- Kneebone, R. (2003). "Simulation in surgical training: educational issues and practical implications." Medical Education, 37(3), 267-277.
- Cook, D. A., Hatala, R., Brydges, R., Zendejas, B., Szostek, J. H., Wang, A. T., ... & Hamstra, S. J. (2011). "Technology-enhanced simulation for health professions education: a systematic review and meta-analysis." JAMA, 306(9), 978-988.
FAQ
What is the primary goal of medical simulation?
The main objective is to create a zero-risk environment where healthcare professionals can practice safely. It bridges the critical gap between theoretical knowledge and practical application, ensuring that comprehensive training translates directly into improved patient outcomes without harming anyone.
Will robots eventually replace human instructors?
No, human educators remain entirely irreplaceable in healthcare. While artificial intelligence and automated software will handle deep data analytics and scenario generation, experienced clinical instructors are essential. They guide emotional debriefings and provide nuanced, empathetic mentorship during highly complex drills.
Is virtual reality effective for surgical preparation?
Yes, it is incredibly effective for spatial awareness and anatomical mapping. However, the best healthcare programs combine VR with physical haptic systems like LapVision. This hybrid approach ensures the surgeon develops both visual recognition and the critical tactile muscle memory required for safe operations.
Immerse yourself in a demo to see how MedVision transforms traditional learning into an engaging, interactive experience
Subscribe for the Latest News!