Virtual Reality in Medicine: Transforming Healthcare Education and Practice
What is Virtual Reality in Medicine?
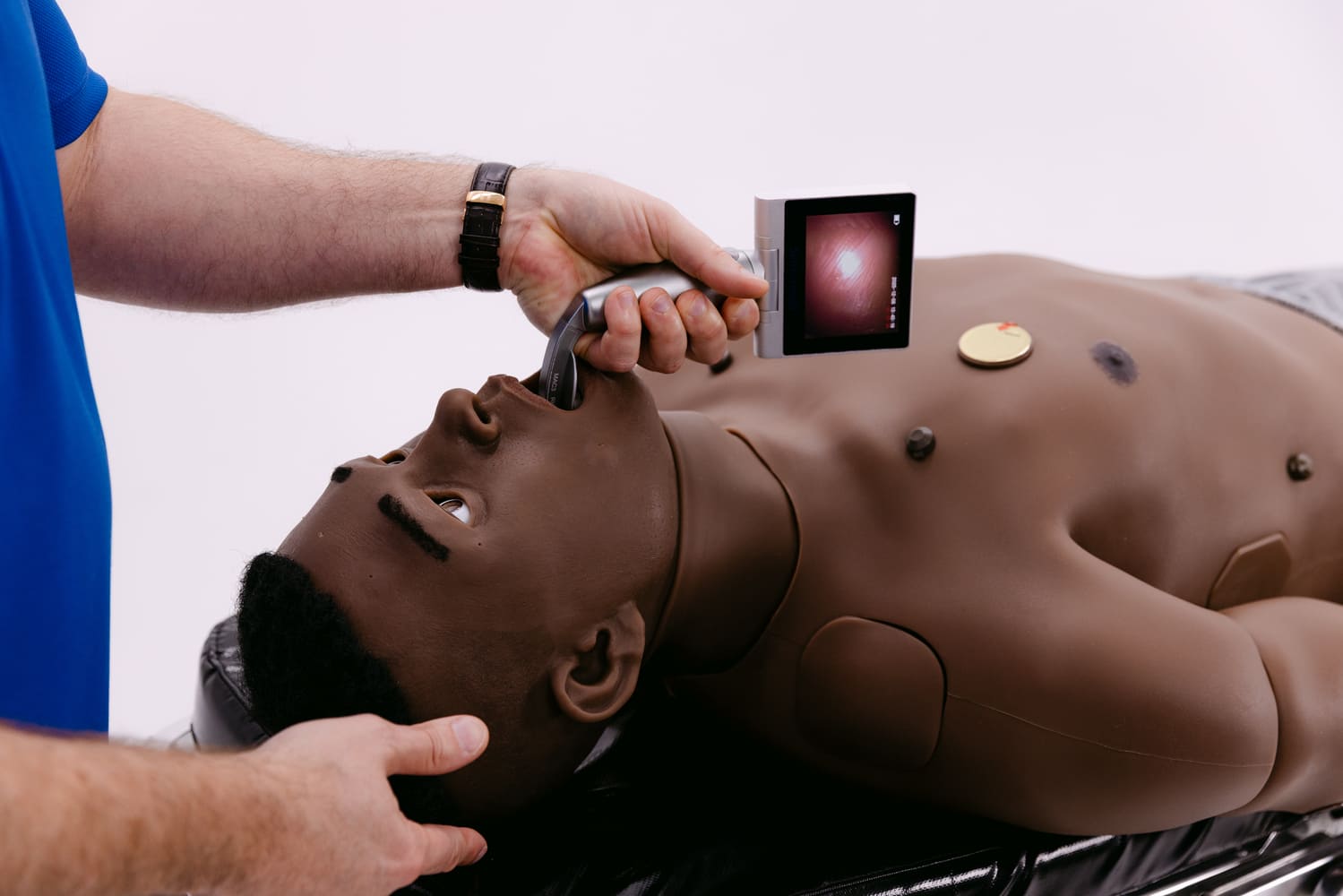
Virtual Reality in Medicine refers to the application of immersive digital environments to support medical training, patient care, and clinical research. Using VR technologies, healthcare professionals can simulate surgical procedures, practice diagnostic skills, and engage in interactive medical education without risk to patients. These technologies are increasingly integrated into healthcare systems to improve safety, efficiency, and outcomes.
Virtual Reality in Medicine encompasses various applications, from preoperative planning to rehabilitation therapies, providing a versatile and safe medical environment. Studies highlight that VR-based interventions enhance learning, retention, and patient engagement, making it a critical tool in modern healthcare education.
Applications of Virtual Reality in Medical Education
One of the most impactful uses of Virtual Reality in medicine is in clinical training. VR simulations allow medical students and practitioners to:
- Perform complex procedures in a controlled environment
- Practice emergency response scenarios without patient risk
- Enhance spatial understanding of anatomy through immersive visualization
- Receive immediate feedback and performance metrics for continuous improvement
By integrating VR into curricula, medical institutions provide a safe and interactive platform for experiential learning, which is essential for competency development in healthcare professions.
Virtual Reality for Surgical Training
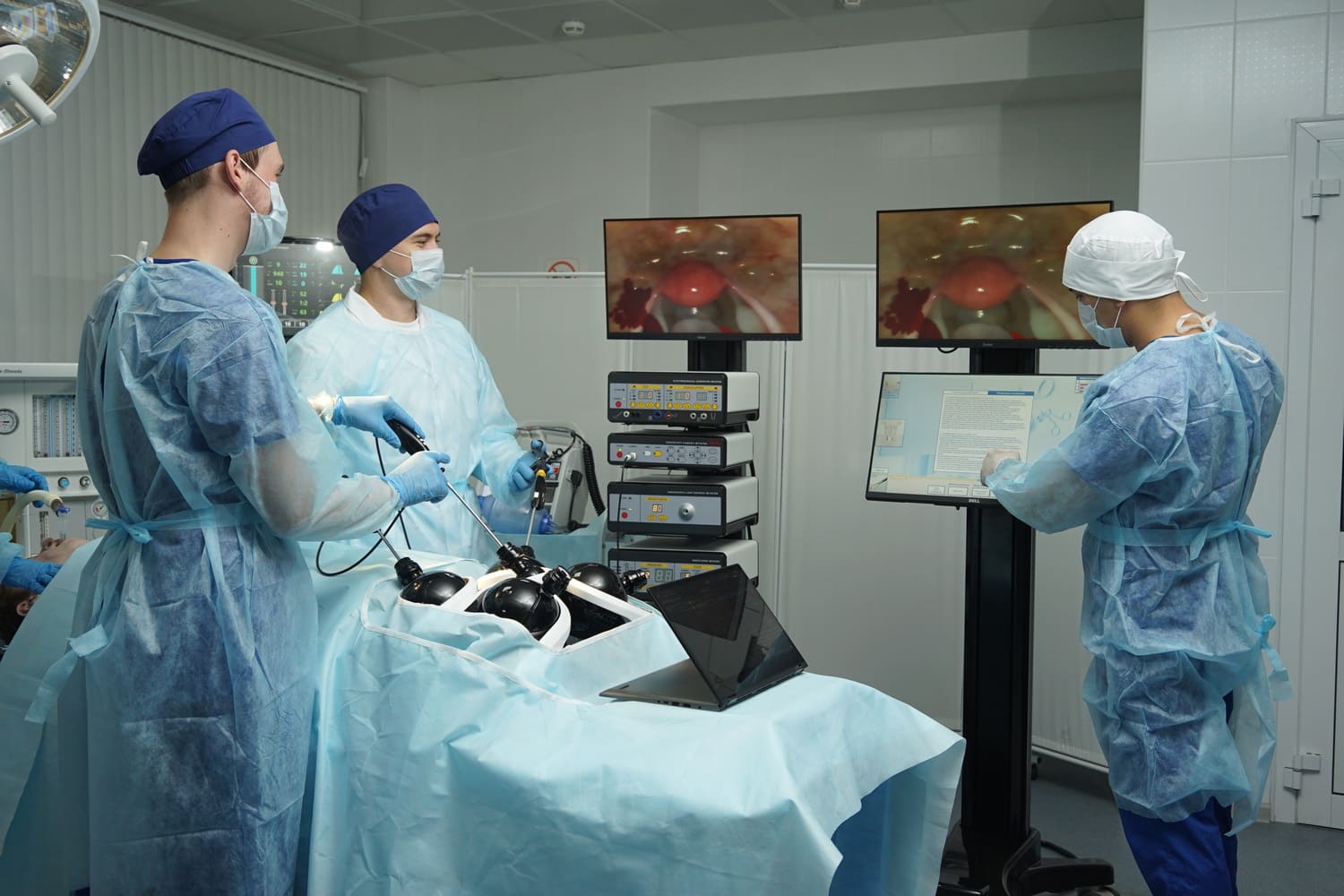
Virtual Reality in Medicine has transformed surgical education. VR simulators replicate operating rooms and patient scenarios, allowing surgeons to rehearse procedures repeatedly. This reduces errors in real surgeries and accelerates skill acquisition. In healthcare, VR-based training is cited as a tool that improves hand-eye coordination, decision-making, and procedural confidence.
Advanced VR platforms provide haptic feedback, realistic anatomical models, and scenario variation, enabling learners to engage with diverse cases. The combination of technology and medical expertise ensures that VR enhances both cognitive and technical competencies.
VR for Patient Treatment and Therapy
Beyond education, Virtual Reality is applied directly to patient care. VR interventions in medicine include:
- Pain management through distraction therapy
- Physical rehabilitation for musculoskeletal injuries
- Treatment of phobias and anxiety disorders
- Cognitive therapy for neurological conditions
These VR applications provide measurable improvements in patient outcomes and satisfaction. By simulating therapeutic environments, patients can engage safely and effectively, making VR a valuable tool in modern healthcare.
VR in Diagnostic Medicine
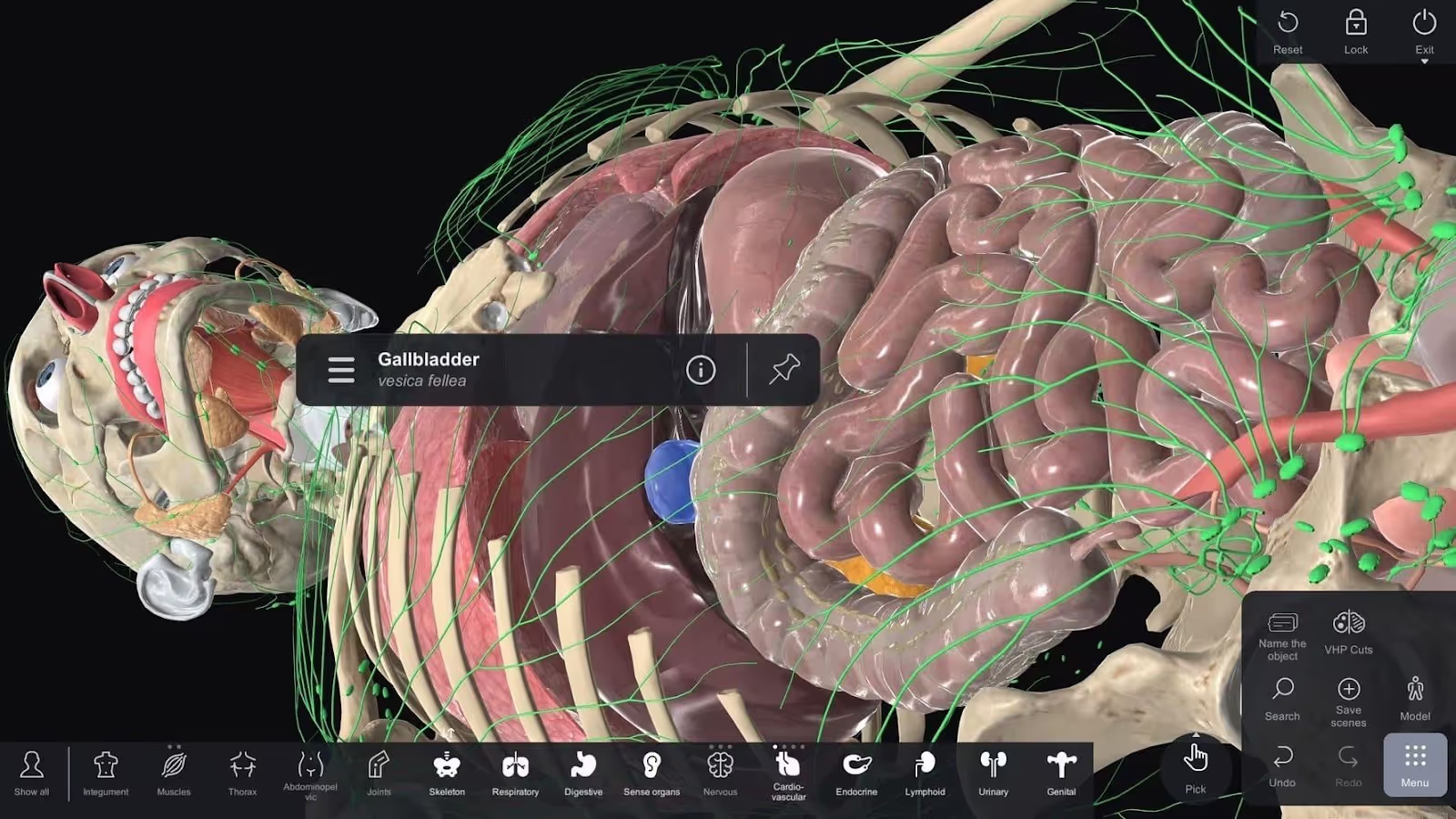
In diagnostic applications, Virtual Reality in Medicine allows physicians to visualize complex anatomical structures and pathological conditions. Interactive 3D models support radiology, cardiology, and neurology, improving medical decision-making. VR-enhanced imaging contributes to precision in diagnosis, early intervention, and treatment planning, creating a safer and more efficient healthcare system.
Virtual Reality for Rehabilitation
Virtual Reality in Medicine is increasingly used for physical and cognitive rehabilitation. Patients recovering from strokes, injuries, or neurological conditions benefit from immersive VR exercises that improve motor skills, balance, and coordination. Customized medical VR programs allow repetitive practice in a controlled environment, enhancing the learning of movement patterns and functional recovery. Clinical studies cited show significant improvements in patient outcomes when VR is integrated into rehabilitation protocols.
Enhancing Medical Training Through VR
Virtual Reality provides medical students and professionals with immersive experiences that traditional methods cannot replicate. VR simulations enable practice of rare or high-risk procedures without danger to patients. This technology supports skill acquisition in surgery, emergency response, and diagnostic testing, making it an essential tool in modern healthcare education. The learning process in VR enhances memory retention and decision-making, ensuring trainees gain practical experience safely.
VR in Pain Management and Mental Health
In addition to education, Virtual Reality in Medicine is applied therapeutically. VR environments distract patients during painful procedures, reducing discomfort and anxiety. Mental health applications include exposure therapy for phobias, stress reduction, and treatment of PTSD. Immersive VR provides a safe and controlled medical environment where patients can interact with therapeutic scenarios, improving engagement and efficacy of treatment in healthcare settings.
Technological Innovations in Medical VR
Advancements in VR hardware and software have expanded its utility in medicine. Haptic devices, motion tracking, and realistic 3D anatomical models allow precise simulation of surgical techniques and patient interactions. Integration with artificial intelligence enables adaptive learning, real-time feedback, and performance analytics. These technological innovations create a sophisticated learning process, making VR a critical tool in both medical education and patient care.
VR for Remote Medical Collaboration
Virtual Reality also facilitates remote collaboration in healthcare. Surgeons and specialists can join VR environments to consult on procedures, review complex cases, or provide guidance during operations. This collaborative approach improves access to expert knowledge, reduces medical errors, and enhances the quality of medicine delivered in geographically diverse locations. VR serves as a powerful medical communication tool in modern healthcare systems.

Improving Patient Education
Virtual Reality in Medicine helps patients understand their conditions and treatments. Immersive VR experiences demonstrate anatomy, surgical procedures, and therapy exercises. This interactive approach increases patient engagement, comprehension, and adherence to medical recommendations. By providing a safe and visual medical environment, VR supports informed decision-making and strengthens the patient-provider relationship in healthcare.
VR in Surgical Planning
Virtual Reality in Medicine allows surgeons to plan complex operations with unprecedented precision. Using 3D patient imaging integrated into VR environments, surgeons can rehearse procedures, anticipate challenges, and optimize surgical strategies. This reduces intraoperative errors, shortens operation times, and enhances patient safety. VR-based planning is increasingly cited in clinical research as a transformative tool for advanced medical practice.
VR in Telemedicine
The integration of Virtual Reality into telemedicine expands access to specialized care. Remote patients can interact with clinicians in immersive environments, allowing for visual examination, rehabilitation exercises, or consultation. This application enhances healthcare delivery in rural and underserved areas, providing high-quality medical attention without travel. VR-enabled telemedicine platforms strengthen both patient engagement and clinical efficiency.
Ethical and Practical Considerations
While Virtual Reality in Medicine offers significant benefits, ethical and practical considerations must be addressed. Privacy of patient data, cost of VR equipment, and training for healthcare providers are critical factors. Institutions implementing VR must establish protocols for secure usage, maintain professional standards, and ensure equitable access. Studies cited highlight that careful integration of VR maximizes benefits while minimizing risks in medical education and patient care.
Future Directions of VR in Medicine
The future of Virtual Reality in Medicine includes AI-driven adaptive learning, advanced haptics, and fully immersive remote surgical platforms. As technology evolves, VR will expand beyond training to real-time procedural support, personalized rehabilitation, and enhanced patient engagement. Continuous innovation in VR ensures that healthcare professionals are better prepared, medical procedures are safer, and patient outcomes improve.
VR for Anatomy Education
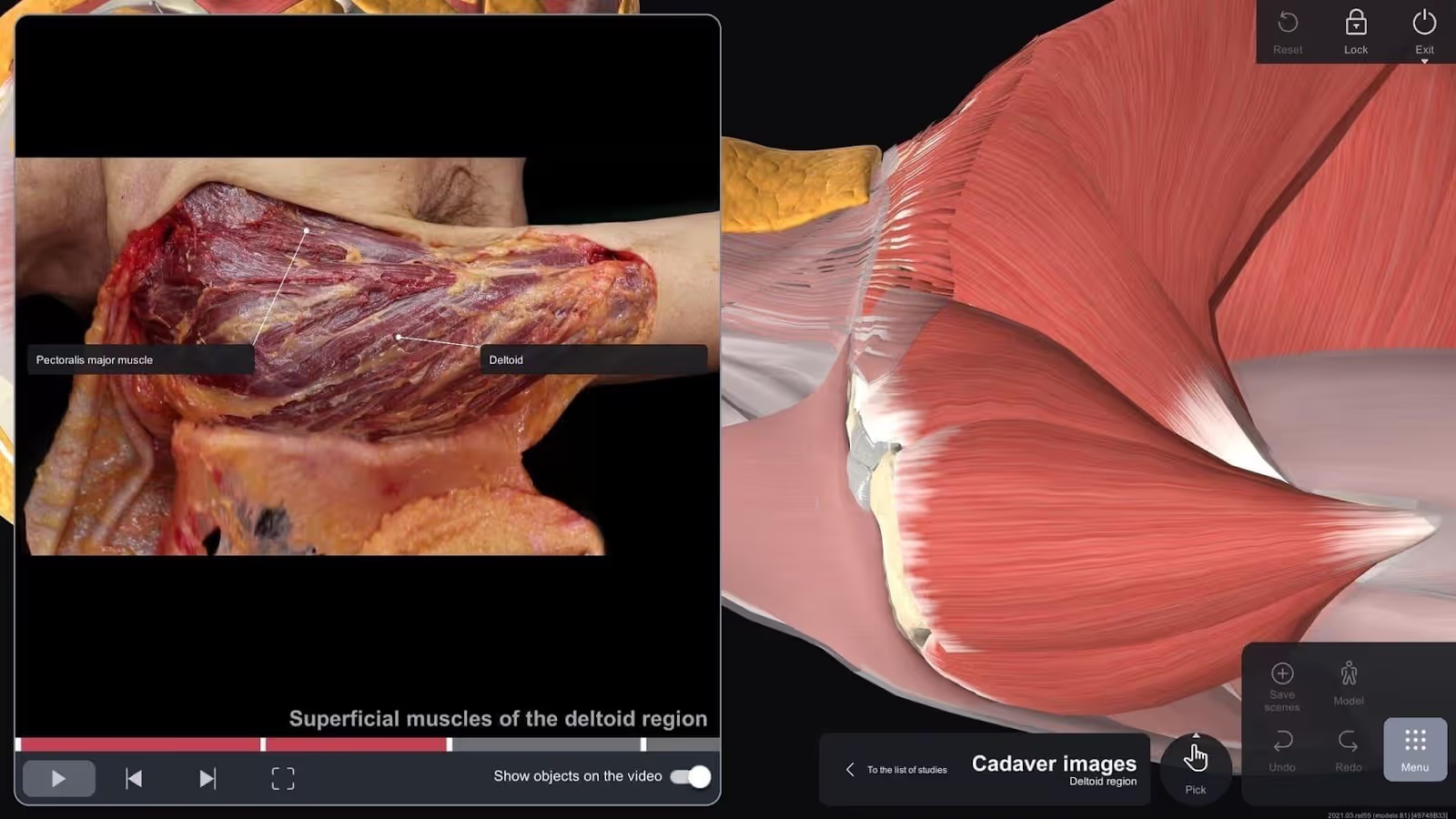
Virtual Reality in Medicine allows students to explore human anatomy interactively. Unlike traditional textbooks or cadaver labs, VR provides a fully immersive medical environment where learners can manipulate organs, visualize structures from different angles, and understand spatial relationships. This enhances comprehension and accelerates the learning process in healthcare education.
VR in Emergency Response Training
Virtual Reality is used to simulate emergency scenarios in medicine. Trainees can practice responses to trauma, cardiac arrest, or mass casualty incidents. By repeating simulation exercises in a controlled environment, healthcare professionals improve decision-making, teamwork, and procedural efficiency. Evidence cited shows VR training reduces errors and prepares staff for real-world emergencies.
VR-Assisted Rehabilitation
Virtual Reality in Medicine supports rehabilitation by providing gamified medical exercises that motivate patients. Stroke survivors, orthopedic patients, and those with neurological conditions perform repetitive tasks in immersive VR settings. This enhances motor recovery, compliance, and engagement. VR platforms track performance, offering clinicians a valuable source of patient progress data.
VR in Pain and Anxiety Management
Pain management is another innovative application of Virtual Reality in medicine. VR environments distract patients during procedures or chronic pain therapy, reducing discomfort and stress. Mental health applications, including exposure therapy for phobias and anxiety disorders, improve outcomes by immersing patients in controlled medical simulations, supporting overall healthcare effectiveness.
VR in Patient Education
Virtual Reality in Medicine is increasingly used to educate patients about procedures and conditions. Patients experience interactive simulations of surgical interventions, rehabilitation exercises, or anatomy explanations. This immersive approach improves comprehension, engagement, and adherence to medical advice, strengthening the learning process and patient-provider communication in healthcare settings.
VR in Remote Medical Collaboration
Virtual Reality allows clinicians from different locations to collaborate in real time. Surgeons can guide procedures, specialists can consult, and multidisciplinary teams can plan treatments in immersive VR spaces. This enhances communication, accelerates decision-making, and improves outcomes in complex medical cases, demonstrating the potential of VR for global healthcare collaboration.
VR in Clinical Research
Virtual Reality in Medicine is applied in clinical research to test new interventions, study patient responses, and simulate scenarios that are otherwise difficult to replicate. VR platforms provide accurate, repeatable simulation environments, generating reliable cited data for research studies. This improves evidence-based practice and advances the scientific understanding of healthcare interventions.
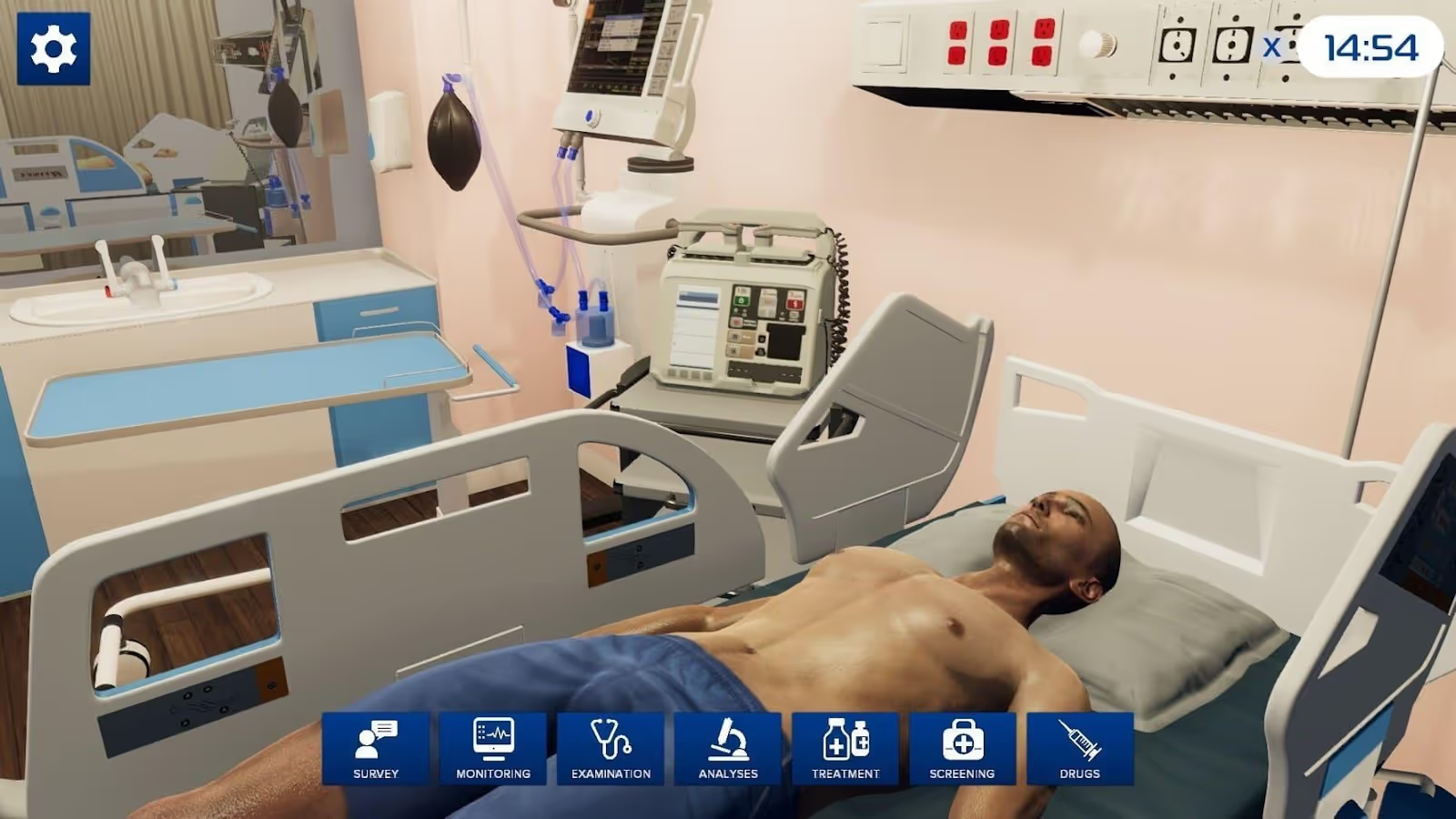
VR for Minimally Invasive Procedures
Virtual Reality helps train clinicians for minimally invasive surgeries, such as laparoscopic or endoscopic procedures. Trainees practice hand-eye coordination, tool manipulation, and spatial awareness within VR medical simulations. These sessions reduce the learning curve, increase confidence, and enhance patient safety in real medicine applications.
VR and Interdisciplinary Training
Virtual Reality in Medicine facilitates interdisciplinary training for nurses, physicians, and allied health professionals. Shared VR scenarios promote teamwork, communication, and understanding of roles. This collaborative learning process prepares healthcare teams for complex situations and enhances overall clinical performance.
VR in Chronic Disease Management
VR interventions support patients with chronic diseases such as diabetes or cardiovascular conditions. Immersive VR programs teach lifestyle modifications, exercise routines, and self-monitoring strategies. Patients engage actively with their medical care plans, improving adherence and outcomes, while clinicians gain a source of continuous data for monitoring progress.
VR for Cognitive Rehabilitation
Virtual Reality in Medicine is used in cognitive rehabilitation for patients with brain injuries, dementia, or neurological deficits. VR exercises enhance memory, attention, and problem-solving skills in a controlled environment. Studies cited show these programs improve cognitive function and quality of life, providing a safe healthcare tool for neurorehabilitation.
VR in Painful Medical Procedures
Virtual Reality reduces stress and discomfort during painful procedures like chemotherapy or wound care. Immersive environments distract patients, lowering perceived pain and anxiety. These VR interventions are increasingly cited as effective adjuncts in medicine, improving patient experience and treatment adherence in clinical healthcare settings.
VR in Medical Imaging
Virtual Reality in Medicine enhances interpretation of complex medical imaging. Clinicians can visualize 3D reconstructions of CT, MRI, or ultrasound data within immersive VR platforms. This improves diagnostic accuracy, procedural planning, and understanding of patient anatomy, supporting safer and more effective medical practice.
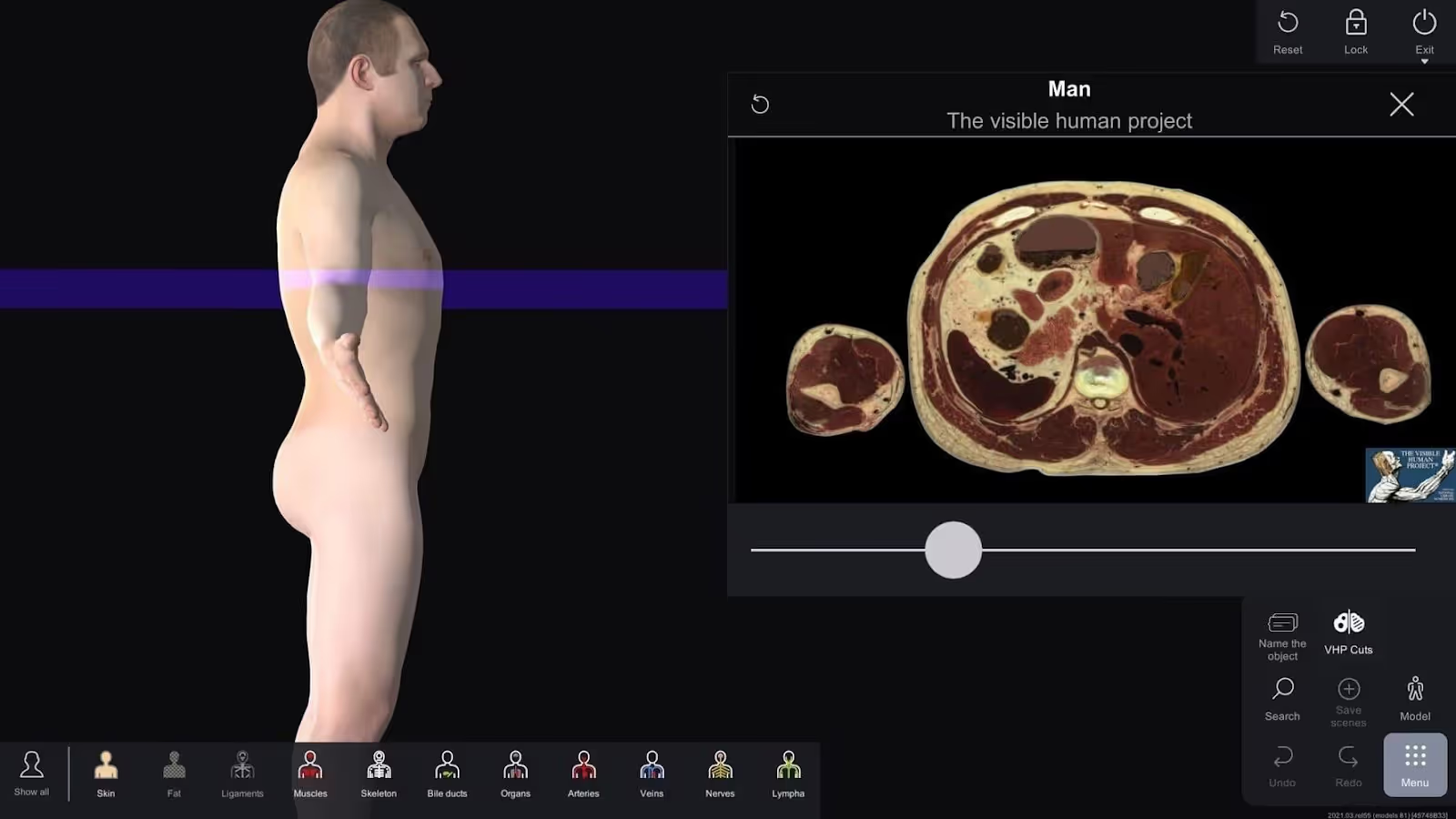
VR for Medical Simulation Assessment
Virtual Reality in Medicine allows educators to assess clinical skills in realistic VR simulations. Trainees perform procedures while facilitators monitor performance metrics, decision-making, and procedural accuracy. This assessment method provides objective data for the learning process and ensures that medical students and professionals meet competency standards in healthcare practice.
VR for Pediatric Care
Virtual Reality is increasingly applied in pediatric medicine. VR environments distract children during painful procedures, provide interactive educational experiences, and reduce anxiety in hospitals. Immersive VR programs improve cooperation, enhance understanding of treatment plans, and make clinical visits less stressful for young patients in healthcare settings.
VR for Remote Surgery Guidance
Virtual Reality in Medicine enables remote surgical guidance, connecting experienced surgeons with trainees across distances. Using immersive VR, mentors can provide step-by-step instructions during procedures, improving training efficiency and patient safety. This approach expands access to expert knowledge and supports skill development in diverse medical environments.
VR in Medical Conferences and Training Workshops
Medical conferences increasingly integrate VR to demonstrate procedures, anatomical models, and clinical innovations. Virtual Reality in medicine allows attendees to experience immersive simulations, enhancing engagement and retention. This approach modernizes professional development and strengthens the learning process across healthcare disciplines.
VR for Neurorehabilitation
Virtual Reality in Medicine plays a key role in neurorehabilitation programs. Patients with stroke, traumatic brain injury, or neurodegenerative disorders engage in immersive exercises that improve motor coordination, cognitive function, and daily living skills. VR-based interventions provide a measurable source of progress data for clinicians while enhancing patient motivation and outcomes.

VR for Pain Distraction During Procedures
In medicine, Virtual Reality is applied to reduce procedural pain. Immersive VR experiences distract patients during treatments such as dental work, chemotherapy, or minor surgeries. Clinical studies cited indicate that VR interventions decrease perceived pain and anxiety, improving patient satisfaction and adherence in healthcare.
VR for Training in Rare Medical Scenarios
Virtual Reality in Medicine allows simulation of rare or high-risk cases that trainees may not encounter frequently. These VR scenarios prepare clinicians to respond confidently to unusual conditions, improving critical thinking, procedural skills, and patient safety. Incorporating VR for rare case training strengthens the overall learning process in medical education.
VR in Tele-rehabilitation
Virtual Reality supports tele-rehabilitation programs for patients unable to attend clinics. Remote VR sessions provide guided exercises, monitor progress, and offer feedback in real-time. This application expands access to rehabilitation, enhances patient engagement, and ensures continuity of care in healthcare environments.
Conclusion
Virtual Reality in Medicine is reshaping how healthcare is delivered, taught, and experienced. By providing immersive environments for training, patient treatment, and clinical planning, VR enhances medical education, supports the learning process, and improves patient safety. Studies cited show significant gains in skill retention, procedural accuracy, and patient engagement. As VR technologies advance, their integration into healthcare systems promises a future where medical practice is more effective, efficient, and interactive.
Immerse yourself in a demo to see how MedVision transforms traditional learning into an engaging, interactive experience
Subscribe for the Latest News!